盐酸莫西沙星 标准
盐酸莫西沙星氯化钠注射液

盐酸莫西沙星氯化钠注射液【药品名称】通用名称:盐酸莫西沙星氯化钠注射液英文名称:Moxifloxacin Hydrochloride and Sodium Chloride Injection【成份】本品主要成份为盐酸莫西沙星,化学名为:1-环丙基-7-[(s,s)-2,8-重氮-二环[4.3.0]壬-8-基]-6-氟-8-甲氧-1,4-二氢-4-氧-3-11奎啉羧酸盐酸盐。
【适应症】成人(≥18岁)上呼吸道和下呼吸道感染,如:急性窦炎、慢性支气管炎急性发作、社区获得性肺炎;以及皮肤和软组织感染。
【用法用量】400 mg qd,口服或静滴90分钟。
疗程:慢性支气管炎急性发作- 5天;社区获得性肺炎:序贯给药(静脉给药后继续口服用药)总疗程为7-14天;急性鼻窦炎- 7天;皮肤和软组织感染- 7天。
最多14天。
【不良反应】在莫西沙星的临床试验中,绝大多数的不良反应为轻中度(约90%),由于不良反应导致停用莫西沙星治疗的病人为36%,序贯治疗(静脉给药后继续口服用药)为5.7%。
根据莫西沙星的临床试验总结出的常见不良反应列表如下:发生率≥1%<10%全身症状:腹痛、头痛、注射部位反应(如水肿/过敏/炎症/疼痛)心血管系统:合并低血钾症患者QT间期延长消化系统:恶心、腹泻、呕吐、消化不良、肝功能化验异常特殊感官:味觉倒错神经系统:头晕发生率≥0.1%<1%全身症状:乏力、念珠菌病、疼痛、不适、胸痛心血管系统:心动过速、高血压、心悸、QT间期延长、静脉炎(注射部位)消化系统:口干、恶心和呕吐、腹胀、便秘、口腔念珠菌病、食欲下降、口腔炎、胃肠功能失调、舌炎、γGT(γ谷氨酰转肽酶)增高血液和淋巴系统:白细胞减少、凝血酶原减少/国际标准化比值增高、嗜酸细胞增多、血小板增多症代谢和营养:淀粉酶增加骨骼肌肉系统:关节痛、肌肉痛神经系统失眠、眩晕、神经质、嗜睡、焦虑、震颤、感觉异常呼吸系统:呼吸困难皮肤和附件:皮疹、瘙痒、多汗泌尿生殖系统:阴道念珠菌病、阴道炎发生率≥0.01%<0.1%全身症状:骨盆疼、面部浮肿、背疼、实验室检验异常、过敏反应、腿疼心血管系统:低血压、血管扩张、外周性水肿消化系统:胃炎、舌变色、吞咽困难、黄疸(主要为胆汁淤积性)、腹泻(难辨梭菌)血液和淋巴系统:凝血活酶减少、凝血酶原增加/国际标准化比值降低、血小板减少、贫血代谢和营养:高血糖、高血脂、高尿酸血症、LDH(乳酸脱氢酶)增高(与肝功能检查异常有关)骨骼肌肉:关节炎、肌腱异常神经系统:幻觉、人格解体、紧张、动作失调、激动不安、健忘症、失语症、情绪不稳定、睡眠障碍、语言障碍、思维异常、感觉减退、梦异常、惊厥、精神错乱、忧郁症呼吸系统:哮喘皮肤和附件:皮疹(斑丘疹、紫癜、脓泡)、荨麻疹特殊感官:耳鸣、视觉异常、味觉丧失、嗅觉倒错(包括嗅觉倒错,嗅觉减低及嗅觉丧失)、弱视泌尿生殖系统:肾功能异常(肌酐或尿素升高)上市后报道的不良反应:发生率≥0.01%<0.1%心血管系统:晕厥发生率<0.01%过敏性:过敏反应、过敏性休克(可危及生命)、血管性水肿(包括喉头水肿;潜在生命危险)消化系统:伪膜性结肠炎(在极少数病例伴有危及生命的并发症),肝炎(主要为胆汁淤积性)肌肉骨胳系统:肌腱断裂皮肤和附件:斯蒂文斯-约翰逊综合征(Stevens-JohnsonSyndrome)神经系统:精神病反应心血管系统:报道在极少数病例尤其是在有严重的潜在性致心律失常条件的病人出现,包括尖端扭转型室速的室性快速性心律失常和心脏停搏。
2023年关于“盐酸莫西沙星注射液”解析

注意事项
1、致残和潜在的不可逆转的严重不良反应,包括肌腱炎和肌腱断裂、周围神经病变和中枢神经系统的影响:使用氟喹诺酮类 药物(包括盐酸莫西沙星),已有报告在同一患者的身体不同器官系统同时发生致残和潜在的不可逆转的严重不良反应,通 常包括:肌腱炎,肌腱断裂,关节痛,肌痛,周围神经病变和中枢神经系统反应(幻觉,焦虑,抑郁,失眠,严重头痛和错 乱)。这些不良反应可发生在使用盐酸莫西沙星后数小时至数周。任何年龄段的患者,之前没有相关风险因素,均有报告发 生这些不良反应。
由于缺乏这些患者的用药经验,本品应避免用于下列患者:
(1)已知QT间期延长;
(2)室性心律失常,包括尖端扭转型,因为QT间期延长可能导致发生这些状况的风险增加;
(3)持续的心律失常状况,如具有临床显著性的心动过缓和急性心肌缺血;
(4)未治疗的低钾血症或低镁血症;
(5)使用抗心律失常IA类药物(例如,奎尼丁、普鲁卡因胺)或III类药物(例如,胺碘酮、索他洛尔);
用法用量
盐酸莫西沙星氯化钠注射液: 盐酸莫西沙星氯化钠注射液用于感染性疾病的治疗,通用的用法用量如下所示,但必须结合疾病严重程度由临床医生最终确定。 4、给药说明: (1)给药前应检查本品是否有不溶颗粒或变色。应使用澄明,无不溶颗粒的本品。穿刺使用前应对本品进行目视检查,不得使用变色、存在颗粒物质或容器存在破损的 产品。 (2)盐酸莫西沙星氯化钠注射液为静脉注射剂,只能用于静脉滴注,不能用于动脉内、肌内、鞘内注射,不能腹膜内或皮下给药。 (3)由于本品与其他注射液的相容性数据较少,本品中不得加入溶媒或其他药物,也不得使用同根静脉输液管同时输注本品,溶媒或其他药物。如使用同根静脉输液管 或Y型管来连续滴注其他药物,或采用背负式输液,在滴注本品之前和之后,应使用和本品和其他滴注药物相容的注射液冲洗该管路。 (4)当开具盐酸莫西沙星来治疗某种细菌感染时,应告知患者:尽管在疗程早期病情通常会好转,但仍应遵医嘱使用药物。跳过剂量或不完成整个疗程可能会降低紧急 治疗的有效性,增加细菌耐药性形成的可能性,未来将不能使用盐酸莫西沙星或其他抗菌药进行治疗。 5、药物相容性:比例在1:10至10:1之间时,本品与下列静脉注射液相容: (1)0.9%氯化钠注射液,无菌注射用水。 (2)1M氯化钠注射液,10%葡萄糖注射液。 (3)5%葡萄糖注射液,乳酸林格注射液 6、种族差异:对高加索人、日本人、黑人及其他种族人群进行了可能的种族间差别试验,未发现临床相关的药代动力学差别。因此,不同种族间不必调整药物剂量。
盐酸莫西沙星片说明书
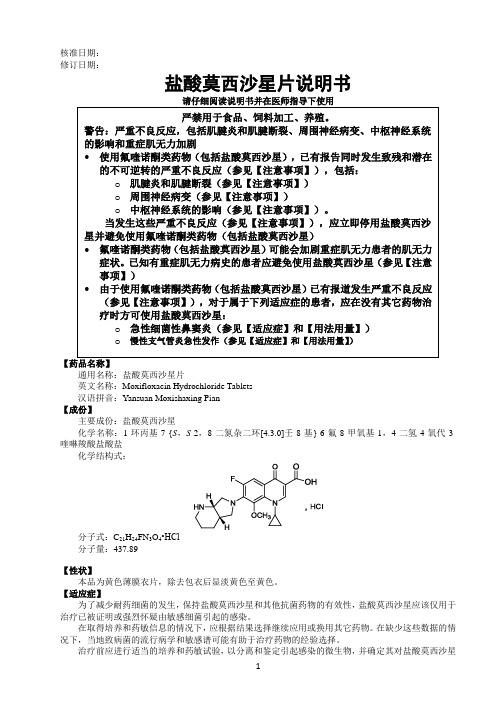
修订日期:盐酸莫西沙星片说明书请仔细阅读说明书并在医师指导下使用通用名称:盐酸莫西沙星片英文名称:Moxifloxacin Hydrochloride Tablets汉语拼音:Yansuan Moxishaxing Pian【成份】主要成份:盐酸莫西沙星化学名称:1-环丙基-7-{S,S-2,8-二氮杂二环[4.3.0]壬-8-基}-6-氟-8-甲氧基-1,4-二氢-4-氧代-3-喹啉羧酸盐酸盐化学结构式:分子式:C21H24FN3O4•HCl分子量:437.89【性状】本品为黄色薄膜衣片,除去包衣后显淡黄色至黄色。
【适应症】为了减少耐药细菌的发生,保持盐酸莫西沙星和其他抗菌药物的有效性,盐酸莫西沙星应该仅用于治疗已被证明或强烈怀疑由敏感细菌引起的感染。
在取得培养和药敏信息的情况下,应根据结果选择继续应用或换用其它药物。
在缺少这些数据的情况下,当地致病菌的流行病学和敏感谱可能有助于治疗药物的经验选择。
治疗前应进行适当的培养和药敏试验,以分离和鉴定引起感染的微生物,并确定其对盐酸莫西沙星在获得培养结果之前可能已经选择盐酸莫西沙星进行治疗,一旦获得培养结果,应选择适当的治疗。
盐酸莫西沙星片剂用于治疗成人(≥18岁)敏感细菌所引起的下列感染:1、急性细菌性鼻窦炎:由肺炎链球菌、流感嗜血杆菌或卡他莫拉菌引起。
由于使用氟喹诺酮类药物(包括盐酸莫西沙星)已有报道发生严重不良反应,且对于一些患者,急性细菌性鼻窦炎有自限性,应在没有其他药物治疗时方可使用盐酸莫西沙星。
2、慢性支气管炎急性发作:由肺炎链球菌、流感嗜血杆菌、副流感嗜血杆菌、肺炎克雷伯菌、甲氧西林敏感的金黄色葡萄球菌或卡他莫拉菌引起。
由于使用氟喹诺酮类药物(包括盐酸莫西沙星)已有报道发生严重不良反应,且对于一些患者,慢性支气管炎急性发作有自限性,应在没有其他药物治疗时方可使用盐酸莫西沙星。
3、社区获得性肺炎:由肺炎链球菌(包括多药耐药株)、流感嗜血杆菌、卡他莫拉菌、甲氧西林敏感的金黄色葡萄球菌、肺炎克雷伯菌、肺炎支原体或肺炎衣原体引起。
莫西沙星的临床应用及不良反应

莫西沙星的临床应用及不良反应作者:石卫东来源:《中国现代医生》2010年第02期[摘要] 目的综述近年来国内外莫西沙星临床应用以及不良反应。
方法查阅近年来相关文献,结合临床莫西沙星的应用,进行归纳总结。
结果莫西沙星对人体多种脏器和某些组织均有不良影响,而胃肠道和中枢神经系统的不良反应发生率占据榜首。
结论通过加强广大医务工作者对莫西沙星不良反应的认识和了解,进而提高合理用药水平。
[关键词] 莫西沙星;临床应用;不良反应[中图分类号] R789.1[文献标识码] A[文章编号] 1673-9701(2010)02-17-02莫西沙星是氟喹诺酮类药物,是近年来临床应用比较广泛的抗菌药物,也是一类较新的合成抗菌药。
但由于这类药物近年来大量的应用使得药物不良反应日益突出,在治愈和挽救患者生命的同时,给患者健康造成不良影响,以至危及人们的生命。
为此,本文就莫西沙星临床合理使用以及常见的不良反应做一综述,以加强广大医务工作者对其不良反应认识,进而提高合理用药水平。
1莫西沙星临床应用状况莫西沙星为第四代新型喹诺酮类抗菌药,化学名称为1-环丙基-7-(S,S)-2,8-重氮-二环[4,3,0]non-8-yl-6-氟-1,4-二氢-4-氧-3喹啉羧酸,临床用其盐酸盐。
于1999年12月获得美国FDA 批准上市,1997年在我国申请临床研究。
其抗菌谱覆盖了全部呼吸道主要致病菌。
对所有常见社区获得性及非典型呼吸道病原菌有很好的抗菌活性,对肠杆菌及其他革兰阴性菌,包括嗜血流感杆菌、卡他莫拉汉菌(包括β-内酰胺酶阳性或阴性菌株)以及嗜血副流感也有效,对大肠杆菌及金葡菌(包括对环丙沙星高度耐药株)的活性等于或高于目前使用的本类药物如氧氟沙星、左氧氟沙星、司帕沙星和曲伐沙星。
莫西沙星是一种安全有效的抗菌药物,常见临床应用如下。
1.1呼吸道感染金建敏等[1]对莫西沙星治疗社区获得性下呼吸道感染老年患者的耐受性和安全性进行了研究。
盐酸莫西沙星氯化钠注射液与利福霉素钠注射液存在配伍禁忌

盐酸莫西沙星氯化钠注射液与利福霉素钠注射液存在配伍禁忌
发表时间:2014-07-10T16:01:07.310Z 来源:《中外健康文摘》2014年第1期供稿作者:俞亚萍王晶欣杨孝亲
[导读] 且要加强药物使用中的临床观察,确保治疗护理工作安全有效。
俞亚萍王晶欣杨孝亲
(江苏省无锡市人民医院 214023)
【中图分类号】R96 【文献标识码】B 【文章编号】1672-5085(2014)01-0256-01
盐酸莫西沙星氯化钠注射液(商品名:拜复乐;规格为250ml;莫西沙星0.4g与氯化钠2.0g)适用于上呼吸道和下呼吸道感染、复杂腹腔感染,是具有广谱活性和杀菌作用的喹诺酮类抗菌素。
利福霉素钠注射液(规格为5ml:0.25g)性状为暗红色的澄清液体,适用于结核杆菌感染的疾病和重症感染的联合治疗。
我科在治疗1例结核性腹膜炎病人中,静脉点滴完盐酸莫西沙星氯化钠注射液250ml后更换5%葡萄糖注射液250ml+利福霉素钠0.5g时输液管内产生暗红色沉淀,立即停止输液,予更换输液器后输注正常,观察患者病情变化,患者未发生输液不良反应。
建议:盐酸莫西沙星氯化钠注射液与利福霉素钠注射液存在配伍禁忌,提示临床上使用此两种药物时中间需加1瓶适合于病情的液体冲管,以免出现药物不良反应,给病人带来不必要的压力。
且要加强药物使用中的临床观察,确保治疗护理工作安全有效。
盐酸莫西沙星氯化钠注射液说明书

AVELOX®(moxifloxacin hydrochloride) TabletsAVELOX® I.V.(moxifloxacin hydrochloride in sodium chloride injection)XXXXXXX, R.X02/08 To reduce the development of drug-resistant bacteria and maintain the effectiveness of AVELOX® and other antibacterial drugs, AVELOX should be used only to treat or prevent infections that are proven or strongly suspected to be caused by bacteria.DESCRIPTIONAVELOX (moxifloxacin hydrochloride) is a synthetic broad spectrum antibacterial agent and is available as AVELOX Tablets for oral administration and as AVELOX I.V. for intravenous administration. Moxifloxacin, a fluoroquinolone, is available as the monohydrochloride salt of 1-cyclopropyl-7-[(S,S)-2,8-diazabicyclo[4.3.0]non-8-yl]-6-fluoro-8-methoxy-1,4-dihydro-4-oxo-3 quinoline carboxylic acid. It is a slightly yellow to yellow crystalline substance with a molecular weight of 437.9. Its empirical formula is C21H24FN3O4 *HCl and its chemical structure is as follows:AVELOX Tablets are available as film-coated tablets containing moxifloxacin hydrochloride (equivalent to 400 mg moxifloxacin). The inactive ingredients are microcrystalline cellulose, lactose monohydrate, croscarmellose sodium, magnesium stearate, hypromellose, titanium dioxide, polyethylene glycol and ferric oxide.AVELOX I.V. is available in ready-to-use 250 mL latex-free flexibags as a sterile, preservative free, 0.8% sodium chloride aqueous solution of moxifloxacin hydrochloride (containing 400 mg moxifloxacin) with pH ranging from 4.1 to 4.6. The appearance of the intravenous solution is yellow. The color does not affect, nor is it indicative of, product stability. The inactive ingredients are sodium chloride, USP, Water for Injection, USP, and may include hydrochloric acid and/or sodium hydroxide for pH adjustment.CLINICAL PHARMACOLOGYAbsorptionMoxifloxacin, given as an oral tablet, is well absorbed from the gastrointestinal tract. The absolute bioavailability of moxifloxacin is approximately 90 percent. Co-administration with a high fat meal (i.e., 500 calories from fat) does not affect the absorption of moxifloxacin. Consumption of 1 cup of yogurt with moxifloxacin does not significantly affect the extent or rate of systemic absorption (AUC).The mean (± SD) C max and AUC values following single and multiple doses of 400 mg moxifloxacin given orally are summarized below.C max (mg/L)AUC(mg•h/L)Half-life(hr)Single Dose OralHealthy (n = 372) 3.1 ± 1.036.1 ± 9.111.5 - 15.6* Multiple Dose OralHealthy young male/female (n = 15) 4.5 ± 0.548.0 ± 2.712.7 ± 1.9 Healthy elderly male (n = 8) 3.8 ± 0.351.8 ± 6.7Healthy elderly female (n = 8) 4.6 ± 0.654.6 ± 6.7Healthy young male (n = 8) 3.6 ± 0.548.2 ± 9.0Healthy young female (n = 9) 4.2 ± 0.549.3 ± 9.5* Range of means from different studiesThe mean (± SD) C max and AUC values following single and multiple doses of 400 mg moxifloxacin given by 1 hour I.V. infusion are summarized below.C max (mg/L)AUC(mg•h/L)Half-life(hr)Single Dose I.V.Healthy young male/female (n = 56) 3.9 ± 0.939.3 ± 8.68.2 - 15.4* Patients (n = 118)Male (n = 64) 4.4 ± 3.7Female (n = 54) 4.5 ± 2.0< 65 years (n = 58) 4.6 ± 4.2≥ 65 years (n = 60) 4.3 ± 1.3Multiple Dose I.V.Healthy young male (n = 8) 4.2 ± 0.838.0 ± 4.714.8 ± 2.2 Healthy elderly (n =12; 8 male, 4 female) 6.1 ± 1.348.2 ± 0.910.1 ± 1.6 Patients** (n = 107)Male (n = 58) 4.2 ± 2.6Female (n = 49) 4.6 ± 1.5< 65 years (n = 52) 4.1 ± 1.4≥ 65 years (n = 55) 4.7 ± 2.7* Range of means from different studies** Expected C max (concentration obtained around the time of the end of the infusion)Plasma concentrations increase proportionately with dose up to the highest dose tested (1200 mg single oral dose). The mean (± SD) elimination half-life from plasma is 12 ± 1.3 hours; steady-state is achieved after at least three days with a 400 mg once daily regimen.Mean Steady-State Plasma Concentrations of Moxifloxacin Obtained With Once Daily Dosing of 400 mg Either Orally (n=10) or by I.V. Infusion (n=12)DistributionMoxifloxacin is approximately 30-50% bound to serum proteins, independent of drug concentration. The volume of distribution of moxifloxacin ranges from 1.7 to 2.7 L/kg. Moxifloxacin is widely distributed throughout the body, with tissue concentrations often exceeding plasma concentrations. Moxifloxacin has been detected in the saliva, nasal and bronchial secretions, mucosa of the sinuses, skin blister fluid, subcutaneous tissue, skeletal muscle, and abdominal tissues and fluids following oral or intravenous administration of 400 mg. Moxifloxacin concentrations measured post-dose in various tissues and fluids following a 400 mg oral or I.V. dose are summarized in the following table. The rates of elimination of moxifloxacin from tissues generally parallel the elimination from plasma.Moxifloxacin Concentrations (mean ± SD) in Tissuesand the Corresponding Plasma Concentrations After a Single 400 mg Oral orIntravenous Dose §Tissue or Fluid NPlasmaConcentration(µg/mL)Tissue or FluidConcentration(µg/mL or µg/g)TissuePlasmaRatio:RespiratoryAlveolar Macrophages5 3.3± 0.761.8± 27.321.2 ± 10.0 Bronchial Mucosa8 3.3± 0.7 5.5± 1.3 1.7 ± 0.3 Epithelial Lining Fluid5 3.3± 0.724.4± 14.78.7 ± 6.1 SinusMaxillary Sinus Mucosa4 3.7± 1.1†7.6± 1.7 2.0 ± 0.3 Anterior Ethmoid Mucosa3 3.7± 1.1†8.8± 4.3 2.2 ± 0.6 Nasal Polyps4 3.7± 1.1†9.8± 4.5 2.6 ± 0.6 Skin, MusculoskeletalBlister Fluid5 3.0± 0.5‡ 2.6± 0.9 0.9 ± 0.2 Subcutaneous Tissue6 2.3± 0.4#0.9± 0.3* 0.4 ± 0.6 Skeletal Muscle6 2.3± 0.4#0.9± 0.2* 0.4 ± 0.1 Intra-AbdominalAbdominal tissue 8 2.9± 0.5 7.6 ± 2.0 2.7 ± 0.8 Abdominal exudate 10 2.3±0.5 3.5 ±1.2 1.6 ± 0.7 Abscess fluid 6 2.7± 0.7 2.3 ±1.5 0.8±0.4§all moxifloxacin concentrations were measured 3 hours after a single 400 mg dose, except the abdominal tissue and exudate concentrations which were measured at 2 hours post-dose and the sinus concentrations which were measured 3 hours post-dose after 5 days of dosing.† N = 5‡N = 7#N = 12* Reflects only non-protein bound concentrations of drug.MetabolismApproximately 52% of an oral or intravenous dose of moxifloxacin is metabolized via glucuronide and sulfate conjugation. The cytochrome P450 system is not involved in moxifloxacin metabolism, and is not affected by moxifloxacin. The sulfate conjugate (M1) accounts for approximately 38% of the dose, and is eliminated primarily in the feces. Approximately 14% of an oral or intravenous dose is converted to a glucuronide conjugate (M2), which is excreted exclusively in the urine. Peak plasma concentrations of M2 are approximately 40% those of the parent drug, while plasma concentrations of M1 are generally less than 10% those of moxifloxacin.In vitro studies with cytochrome (CYP) P450 enzymes indicate that moxifloxacin does not inhibit CYP3A4, CYP2D6, CYP2C9, CYP2C19, or CYP1A2, suggesting that moxifloxacin is unlikely to alter the pharmacokinetics of drugs metabolized by these enzymes.ExcretionApproximately 45% of an oral or intravenous dose of moxifloxacin is excreted as unchanged drug (~20% in urine and ~25% in feces). A total of 96% ± 4% of an oral dose is excreted as either unchanged drug or known metabolites. The mean (± SD) apparent total body clearance and renal clearance are 12 ± 2.0 L/hr and 2.6 ± 0.5 L/hr, respectively.Special PopulationsGeriatricFollowing oral administration of 400 mg moxifloxacin for 10 days in 16 elderly (8 male; 8 female) and 17 young (8 male; 9 female) healthy volunteers, there were no age-related changes in moxifloxacin pharmacokinetics. In 16 healthy male volunteers (8 young; 8 elderly) given a single 200 mg dose of oral moxifloxacin, the extent of systemic exposure (AUC and C max)was not statistically different between young and elderly males and elimination half-life was unchanged. No dosage adjustment is necessary based on age. In large phase III studies, the concentrations around the time of the end of the infusion in elderly patients following intravenous infusion of 400 mg were similar to those observed in young patients.PediatricThe pharmacokinetics of moxifloxacin in pediatric subjects have not been studied.GenderFollowing oral administration of 400 mg moxifloxacin daily for 10 days to 23 healthy males (19-75 years) and 24 healthy females (19-70 years), the mean AUC and C max were 8% and 16% higher, respectively, in females compared to males. There are no significant differences in moxifloxacin pharmacokinetics between male and female subjects when differences in body weight are taken into consideration.A 400 mg single dose study was conducted in 18 young males and females. The comparison of moxifloxacin pharmacokinetics in this study (9 young females and 9 young males) showed no differences in AUC or C max due to gender. Dosage adjustments based on gender are not necessary. RaceSteady-state moxifloxacin pharmacokinetics in male Japanese subjects were similar to those determined in Caucasians, with a mean C max of 4.1 µg/mL, an AUC24 of 47 µg•h/mL, and an elimination half-life of 14 hours, following 400 mg p.o. daily.Renal InsufficiencyThe pharmacokinetic parameters of moxifloxacin are not significantly altered in mild, moderate, severe, or end-stage renal disease. No dosage adjustment is necessary in patients with renal impairment, including those patients requiring hemodialysis (HD) or continuous ambulatory peritoneal dialysis (CAPD).In a single oral dose study of 24 patients with varying degrees of renal function from normal to severely impaired, the mean peak concentrations (C max) of moxifloxacin were reduced by 21% and 28% in the patients with moderate (CL CR ≥30 and ≤ 60 mL/min) and severe (CL CR < 30 mL/min) renal impairment, respectively. The mean systemic exposure (AUC) in these patients was increased by 13%. In the moderate and severe renally impaired patients, the mean AUC for the sulfate conjugate (M1) increased by 1.7-fold (ranging up to 2.8-fold) and mean AUC andC max for the glucuronide conjugate (M2) increased by 2.8-fold (ranging up to 4.8-fold) and1.4-fold (ranging up to2.5-fold), respectively.The pharmacokinetics of single dose and multiple dose moxifloxacin were studied in patients with CL CR < 20 mL/min on either hemodialysis or continuous ambulatory peritoneal dialysis (8 HD, 8 CAPD). Following a single 400 mg oral dose, the AUC of moxifloxacin in these HD and CAPD patients did not vary significantly from the AUC generally found in healthy volunteers. C max values of moxifloxacin were reduced by about 45% and 33% in HD and CAPD patients, respectively, compared to healthy, historical controls. The exposure (AUC) to the sulfate conjugate (M1) increased by 1.4- to 1.5-fold in these patients. The mean AUC of the glucuronide conjugate (M2) increased by a factor of 7.5, whereas the mean C max values of the glucuronide conjugate (M2) increased by a factor of 2.5 to 3, compared to healthy subjects. The sulfate and the glucuronide conjugates of moxifloxacin are not microbiologically active, and the clinical implication of increased exposure to these metabolites in patients with renal disease including those undergoing HD and CAPD has not been studied.Oral administration of 400 mg QD moxifloxacin for 7 days to patients on HD or CAPD produced mean systemic exposure (AUC ss) to moxifloxacin similar to that generally seen in healthy volunteers. Steady-state C max values were about 22% lower in HD patients but were comparable between CAPD patients and healthy volunteers. Both HD and CAPD removed only small amounts of moxifloxacin from the body (approximately 9% by HD, and 3% by CAPD). HD and CAPD also removed about 4% and 2% of the glucuronide metabolite (M2), respectively. Hepatic InsufficiencyIn 400 mg single oral dose studies in 6 patients with mild (Child Pugh Class A), and 10 patients with moderate (Child Pugh Class B), hepatic insufficiency, moxifloxacin mean systemic exposure (AUC) was 78% and 102%, respectively, of 18 healthy controls and mean peak concentration (C max)was 79% and 84% of controls.The mean AUC of the sulfate conjugate of moxifloxacin (M1) increased by 3.9-fold (ranging up to 5.9-fold) and 5.7-fold (ranging up to 8.0-fold) in the mild and moderate groups, respectively. The mean C max of M1 increased by approximately 3-fold in both groups (ranging up to 4.7- and 3.9-fold). The mean AUC of the glucuronide conjugate of moxifloxacin (M2) increased by 1.5-fold (ranging up to 2.5-fold) in both groups. The mean C max of M2 increased by 1.6- and 1.3-fold (ranging up to 2.7- and 2.1-fold), respectively. The clinical significance of increased exposure to the sulfate and glucuronide conjugates has not been studied. No dosage adjustment is recommended for mild or moderate hepatic insufficiency (Child Pugh Classes A and B). The pharmacokinetics of moxifloxacin in severe hepatic insufficiency (Child Pugh Class C) have not been studied. (See DOSAGE AND ADMINISTRATION.)Photosensitivity PotentialA study of the skin response to ultraviolet (UVA and UVB) and visible radiation conducted in 32 healthy volunteers (8 per group) demonstrated that moxifloxacin does not show phototoxicity in comparison to placebo. The minimum erythematous dose (MED) was measured before and after treatment with moxifloxacin (200 mg or 400 mg once daily), lomefloxacin (400 mg once daily), or placebo. In this study, the MED measured for both doses of moxifloxacin were not significantly different from placebo, while lomefloxacin significantly lowered the MED. (See PRECAUTIONS, Information for Patients.)It is difficult to ascribe relative photosensitivity/phototoxicity among various fluoroquinolones during actual patient use because other factors play a role in determining a subject’s susceptibility to this adverse event such as: a patient’s skin pigmentation, frequency and duration of sun and artificial ultraviolet light (UV) exposure, wearing of sunscreen andprotective clothing, the use of other concomitant drugs and the dosage and duration of fluoroquinolone therapy (See ADVERSE REACTIONS and ADVERSEREACTIONS/Post-Marketing Adverse Event Reports).Drug-drug InteractionsThe potential for pharmacokinetic drug interactions between moxifloxacin and itraconazole, theophylline, warfarin, digoxin, atenolol, probenecid, morphine, oral contraceptives, ranitidine, glyburide, calcium, iron, and antacids has been evaluated. There was no clinically significant effect of moxifloxacin on itraconazole, theophylline, warfarin, digoxin, atenolol, oral contraceptives, or glyburide kinetics. Itraconazole, theophylline, warfarin, digoxin, probenecid, morphine, ranitidine, and calcium did not significantly affect the pharmacokinetics of moxifloxacin. These results and the data from in vitro studies suggest that moxifloxacin is unlikely to significantly alter the metabolic clearance of drugs metabolized by CYP3A4, CYP2D6, CYP2C9, CYP2C19, or CYP1A2 enzymes.As with all other quinolones, iron and antacids significantly reduced bioavailability of moxifloxacin.Itraconazole:In a study involving 11 healthy volunteers, there was no significant effect of itraconazole (200 mg once daily for 9 days), a potent inhibitor of cytochrome P4503A4, on the pharmacokinetics of moxifloxacin (a single 400 mg dose given on the 7th day of itraconazole dosing). In addition, moxifloxacin was shown not to affect the pharmacokinetics of itraconazole. Theophylline:No significant effect of moxifloxacin (200 mg every twelve hours for 3 days) on the pharmacokinetics of theophylline (400 mg every twelve hours for 3 days) was detected in a study involving 12 healthy volunteers. In addition, theophylline was not shown to affect the pharmacokinetics of moxifloxacin. The effect of co-administration of a 400 mg dose of moxifloxacin with theophylline has not been studied, but it is not expected to be clinically significant based on in vitro metabolic data showing that moxifloxacin does not inhibit the CYP1A2 isoenzyme.Warfarin:No significant effect of moxifloxacin (400 mg once daily for eight days) on the pharmacokinetics of R- and S-warfarin (25 mg single dose of warfarin sodium on the fifth day) was detected in a study involving 24 healthy volunteers. No significant change in prothrombin time was observed. (See PRECAUTIONS, Drug Interactions.)Digoxin:No significant effect of moxifloxacin (400 mg once daily for two days) on digoxin (0.6 mg as a single dose) AUC was detected in a study involving 12 healthy volunteers. The mean digoxin C max increased by about 50% during the distribution phase of digoxin. This transient increase in digoxin C max is not viewed to be clinically significant. Moxifloxacin pharmacokinetics were similar in the presence or absence of digoxin. No dosage adjustment for moxifloxacin or digoxin is required when these drugs are administered concomitantly. Atenolol:In a crossover study involving 24 healthy volunteers (12 male; 12 female), the mean atenolol AUC following a single oral dose of 50 mg atenolol with placebo was similar to that observed when atenolol was given concomitantly with a single 400 mg oral dose of moxifloxacin. The mean C max of single dose atenolol decreased by about 10% following co-administration with a single dose of moxifloxacin.Morphine:No significant effect of morphine sulfate (a single 10 mg intramuscular dose) on the mean AUC and C max of moxifloxacin (400 mg single dose) was observed in a study of 20 healthy male and female volunteers.Oral Contraceptives:A placebo-controlled study in 29 healthy female subjects showed that moxifloxacin 400 mg daily for 7 days did not interfere with the hormonal suppression of oral contraception with 0.15 mg levonorgestrel/0.03 mg ethinylestradiol (as measured by serum progesterone, FSH, estradiol, and LH), or with the pharmacokinetics of the administered contraceptive agents.Probenecid:Probenecid (500 mg twice daily for two days) did not alter the renal clearance and total amount of moxifloxacin (400 mg single dose) excreted renally in a study of 12 healthy volunteers.Ranitidine:No significant effect of ranitidine (150 mg twice daily for three days as pretreatment) on the pharmacokinetics of moxifloxacin (400 mg single dose) was detected in a study involving 10 healthy volunteers.Antidiabetic agents:In diabetics, glyburide (2.5 mg once daily for two weeks pretreatment and for five days concurrently) mean AUC and C max were 12% and 21% lower, respectively, when taken with moxifloxacin (400 mg once daily for five days) in comparison to placebo. Nonetheless, blood glucose levels were decreased slightly in patients taking glyburide and moxifloxacin in comparison to those taking glyburide alone, suggesting no interference by moxifloxacin on the activity of glyburide. These interaction results are not viewed as clinically significant. Calcium:Twelve healthy volunteers were administered concomitant moxifloxacin (single 400 mg dose) and calcium (single dose of 500 mg Ca++ dietary supplement) followed by an additional two doses of calcium 12 and 24 hours after moxifloxacin administration. Calcium had no significant effect on the mean AUC of moxifloxacin. The mean C max was slightly reduced and the time to maximum plasma concentration was prolonged when moxifloxacin was given with calcium compared to when moxifloxacin was given alone (2.5 hours versus 0.9 hours). These differences are not considered to be clinically significant.Antacids:When moxifloxacin (single 400 mg tablet dose) was administered two hours before, concomitantly, or 4 hours after an aluminum/magnesium-containing antacid (900 mg aluminum hydroxide and 600 mg magnesium hydroxide as a single oral dose) to 12 healthy volunteers there was a 26%, 60% and 23% reduction in the mean AUC of moxifloxacin, respectively. Moxifloxacin should be taken at least 4 hours before or 8 hours after antacids containing magnesium or aluminum, as well as sucralfate, metal cations such as iron, and multivitamin preparations with zinc, or VIDEX® (didanosine) chewable/ buffered tablets or the pediatric powder for oral solution. (See PRECAUTIONS, Drug Interactions and DOSAGE AND ADMINISTRATION.) Iron:When moxifloxacin tablets were administered concomitantly with iron (ferrous sulfate 100 mg once daily for two days), the mean AUC and C max of moxifloxacin was reduced by 39% and 59%, respectively. Moxifloxacin should only be taken more than 4 hours before or 8 hours after iron products. (See PRECAUTIONS, Drug Interactions and DOSAGE AND ADMINISTRATION.) Electrocardiogram:Prolongation of the QT interval in the ECG has been observed in some patients receiving moxifloxacin. Following oral dosing with 400 mg of moxifloxacin the mean (± SD) change in QTc from the pre-dose value at the time of maximum drug concentration was 6 msec (± 26) (n = 787). Following a course of daily intravenous dosing (400 mg; 1 hour infusion each day) the mean change in QTc from the Day 1 pre-dose value was 9 msec (± 24) on Day 1 (n = 69) and 3 msec (± 29) on Day 3 (n = 290). (See WARNINGS.)There is limited information available on the potential for a pharmacodynamic interaction in humans between moxifloxacin and other drugs that prolong the QTc interval of the electrocardiogram. Sotalol, a Class III antiarrhythmic, has been shown to further increase the QTc interval when combined with high doses of intravenous (I.V.) moxifloxacin in dogs. Therefore, moxifloxacin should be avoided with Class IA and Class III antiarrhythmics. (See ANIMAL PHARMACOLOGY, WARNINGS,and PRECAUTIONS.)MICROBIOLOGYMoxifloxacin has in vitro activity against a wide range of Gram-positive and Gram-negative microorganisms. The bactericidal action of moxifloxacin results from inhibition of the topoisomerase II (DNA gyrase) and topoisomerase IV required for bacterial DNA replication, transcription, repair, and recombination. It appears that the C8-methoxy moiety contributes to enhanced activity and lower selection of resistant mutants of Gram-positive bacteria compared to the C8-H moiety. The presence of the bulky bicycloamine substituent at the C-7 position prevents active efflux, associated with the NorA or pmrA genes seen in certain Gram-positive bacteria. The mechanism of action for quinolones, including moxifloxacin, is different from that of macrolides, beta-lactams, aminoglycosides, or tetracyclines; therefore, microorganisms resistant to these classes of drugs may be susceptible to moxifloxacin and other quinolones. There is no known cross-resistance between moxifloxacin and other classes of antimicrobials.In vitro resistance to moxifloxacin develops slowly via multiple-step mutations. Resistance to moxifloxacin occurs in vitro at a general frequency of between 1.8 x 10–9 to < 1 x 10–11 for Gram-positive bacteria.Cross-resistance has been observed between moxifloxacin and other fluoroquinolones against Gram-negative bacteria. Gram-positive bacteria resistant to other fluoroquinolones may, however, still be susceptible to moxifloxacin.Moxifloxacin has been shown to be active against most strains of the following microorganisms, both in vitro and in clinical infections as described in the INDICATIONS AND USAGE section. Aerobic Gram-positive microorganismsEnterococcus faecalis (many strains are only moderately susceptible)Staphylococcus aureus (methicillin-susceptible strains only)Streptococcus anginosusStreptococcus constellatusStreptococcus pneumoniae (including multi-drug resistant strains [MDRSP]*) Streptococcus pyogenes* MDRSP, Multi-drug resistant Streptococcus pneumoniae includes isolates previously known as PRSP (Penicillin-resistant S. pneumoniae), and are strains resistant to two or more of the following antibiotics: penicillin (MIC ≥ 2 μg/mL), 2nd generation cephalosporins (e.g., cefuroxime), macrolides, tetracyclines, and trimethoprim/sulfamethoxazole.Aerobic Gram-negative microorganismsEnterobacter cloacaeEscherichia coliHaemophilus influenzaeHaemophilus parainfluenzaeKlebsiella pneumoniaeMoraxella catarrhalisProteus mirabilisAnaerobic microorganismsBacteroides fragilisBacteroides thetaiotaomicronClostridium perfringensPeptostreptococcus speciesOther microorganismsChlamydia pneumoniaeMycoplasma pneumoniaeThe following in vitro data are available, but their clinical significance is unknown.Moxifloxacin exhibits in vitro minimum inhibitory concentrations (MICs) of 2 µg/mL or lessagainst most (≥ 90%) strains of the following microorganisms; however, the safety andeffectiveness of moxifloxacin in treating clinical infections due to these microorganisms have notbeen established in adequate and well-controlled clinical trials.Aerobic Gram-positive microorganismsStaphylococcus epidermidis (methicillin-susceptible strains only)Streptococcus agalactiaeStreptococcus viridans groupAerobic Gram-negative microorganismsCitrobacter freundiiKlebsiella oxytocaLegionella pneumophilaAnaerobic microorganismsFusobacterium speciesPrevotella speciesSusceptibility TestsDilution Techniques:Quantitative methods are used to determine antimicrobial minimuminhibitory concentrations (MICs). These MICs provide estimates of the susceptibility of bacteriato antimicrobial compounds. The MICs should be determined using a standardized procedure.Standardized procedures are based on a dilution method1 (broth or agar) or equivalent withstandardized inoculum concentrations and standardized concentrations of moxifloxacin powder.The MIC values should be interpreted according to the following criteria:For testing Enterobacteriaceae and methicillin-susceptible Staphylococcus aureus:MIC (µg/mL)Interpretation≤2.0 Susceptible(S)4.0Intermediate(I)≥8.0Resistant(R)For testing Haemophilus influenzae and Haemophilus parainfluenzae a:MIC (µg/mL) Interpretation(S) ≤1.0 Susceptiblea This interpretive standard is applicable only to broth microdilution susceptibility tests withHaemophilus influenzae and Haemophilus parainfluenzae using Haemophilus Test Medium1.The current absence of data on resistant strains precludes defining any results other than“Susceptible”. Strains yielding MIC results suggestive of a “nonsusceptible” category should besubmitted to a reference laboratory for further testing.For testing Streptococcus species including Streptococcus pneumoniae b and Enterococcus faecalis:MIC (µg/mL)Interpretation≤1.0 Susceptible(S)2.0Intermediate(I)≥ 4.0Resistant(R)b These interpretive standards are applicable only to broth microdilution susceptibility tests using cation-adjusted Mueller-Hinton broth with 2 - 5% lysed horse blood.A report of “Susceptible” indicates that the pathogen is likely to be inhibited if the antimicrobial compound in the blood reaches the concentrations usually achievable. A report of “Intermediate” indicates that the result should be considered equivocal, and, if the microorganism is not fully susceptible to alternative, clinically feasible drugs, the test should be repeated. This category implies possible clinical applicability in body sites where the drug is physiologically concentrated or in situations where a high dosage of drug can be used. This category also provides a buffer zone which prevents small uncontrolled technical factors from causing major discrepancies in interpretation. A report of “Resistant” indicates that the pathogen is not likely to be inhibited if the antimicrobial compound in the blood reaches the concentrations usually achievable; other therapy should be selected.Standardized susceptibility test procedures require the use of laboratory control microorganisms to control the technical aspects of the laboratory procedures. Standard moxifloxacin powder should provide the following MIC values:Microorganism MIC (µg/mL)Enterococcus faecalis ATCC 292120.06- 0.5Escherichia coli ATCC 259220.008- 0.06Haemophilus influenzae ATCC 49247c0.008- 0.03Staphylococcus aureus ATCC 292130.015- 0.06Streptococcus pneumoniae ATCC 49619d0.06- 0.25c This quality control range is applicable to only H. influenzae ATCC 49247 tested by a broth microdilution procedure using Haemophilus Test Medium (HTM)1.d This quality control range is applicable to only S. pneumoniae ATCC 49619 tested by a broth microdilution procedure using cation-adjusted Mueller-Hinton broth with 2 - 5% lysed horse blood.Diffusion Techniques:Quantitative methods that require measurement of zone diameters also provide reproducible estimates of the susceptibility of bacteria to antimicrobial compounds. One such standardized procedure2 requires the use of standardized inoculum concentrations. This procedure uses paper disks impregnated with 5-µg moxifloxacin to test the susceptibility of microorganisms to moxifloxacin.Reports from the laboratory providing results of the standard single-disk susceptibility test with a 5-µg moxifloxacin disk should be interpreted according to the following criteria:。
盐酸莫西沙星的溶解度曲线

盐酸莫西沙星的溶解度曲线盐酸莫西沙星是一种广谱抗生素,常用于治疗呼吸道、泌尿道、消化道等感染疾病。
溶解度曲线是指在不同温度下,溶液中盐酸莫西沙星的溶解度随着溶液浓度的变化而变化的曲线。
下面我们将详细介绍盐酸莫西沙星的溶解度曲线。
首先,先了解一下溶解度的概念。
溶解度是指在一定温度下,溶质在溶剂中达到饱和状态时,单位体积溶液中最多可以溶解的溶质的质量。
溶解度与温度、压力、溶质和溶剂性质有关。
盐酸莫西沙星是一种弱酸性物质,其盐酸盐在水中溶解度随温度的升高而增加。
通常情况下,溶解度曲线是通过实验得出的,记录了不同温度下溶液中盐酸莫西沙星的溶解度。
实验中,一般采用恒温槽和恒温电热板来控制溶液温度,利用酸碱滴定法、紫外分光光度法、体积分析等方法测定溶质在溶剂中的溶解度。
通过测定不同温度下的溶解度,可以得到溶解度曲线。
溶解度曲线通常是以温度为横轴,溶解度为纵轴进行绘制的。
在绘制曲线的过程中,需要进行多组实验,将实验测得的溶质质量与溶液体积的数据进行计算、统计和分析,然后绘制曲线图。
溶解度曲线的形状取决于溶质和溶剂的性质。
对于盐酸莫西沙星溶解度曲线来说,一般呈现出正相关的趋势,即随着温度的升高,溶解度也会增大。
这是因为在较高温度下,溶剂分子的动能较大,分子间相互作用力较小,有利于溶质分子进入溶剂中并与溶剂分子相互作用。
然而,溶解度曲线并非总是呈现单调递增的趋势。
在某些特殊情况下,可能会出现饱和溶解度或溶解度饱和的现象。
这是因为随着温度的升高,溶剂分子的动能达到一定程度后,分子间相互作用力开始增大,溶剂分子将不再与溶质分子相互作用,从而达到溶解度饱和。
除了温度,其他因素如压力、PH值等也会对溶解度曲线产生影响。
此外,还有一些其他因素,如溶剂选择、溶质浓度、表面活性剂等也会对溶解度曲线造成一定的影响。
总结来说,盐酸莫西沙星的溶解度曲线是通过实验测定不同温度下溶液中盐酸莫西沙星的溶解度得出的。
通常情况下,溶解度随温度的升高而增加。
盐酸莫西沙星的溶解度曲线

盐酸莫西沙星的溶解度曲线
盐酸莫西沙星是一种广谱抗菌药,其化学名称为1-环丙基-7-氯-8-氟-1,4-二氢-4-氧-喹啉酸盐酸盐。
盐酸莫西沙星具有较好的抗菌活性,对许多革兰氏阳性菌、革兰氏阴性菌、肺炎支原体、肺炎衣原体和螺旋体等均有较强的抑制作用。
因此,盐酸莫西沙星在医学领域具有广泛的应用。
盐酸莫西沙星的溶解度曲线研究具有重要的实际意义。
溶解度是衡量药物在介质中可溶性的一种指标,关系到药物的生物利用度和疗效。
通过对盐酸莫西沙星溶解度曲线的研究,可以为药物的生产、制剂和临床应用提供科学依据。
盐酸莫西沙星的溶解度曲线具有以下特点:
1.随着温度的升高,盐酸莫西沙星的溶解度逐渐增大。
这说明温度对盐酸莫西沙星的溶解度有正向影响。
2.盐酸莫西沙星的溶解度曲线呈现出典型的S型,表明其在一定范围内溶解度与浓度呈正相关,超过一定浓度后,溶解度增长速度减缓。
3.在pH值为6.5左右时,盐酸莫西沙星的溶解度达到最大。
这说明溶液的酸碱性对药物溶解度有一定影响。
盐酸莫西沙星溶解度曲线在实际应用中的重要性体现在以下几点:
1.生产工艺优化:通过研究溶解度曲线,可以为盐酸莫西沙星的生产工艺提供依据,如选择合适的原料、优化生产条件和工艺流程等。
2.药物制剂:了解盐酸莫西沙星的溶解度特性,有助于开发其固体分散物、缓释制剂等,提高药物的生物利用度和疗效。
3.临床应用:掌握盐酸莫西沙星在不同条件下的溶解度,有助于指导患者如何正确用药,避免药物不良反应。
总之,盐酸莫西沙星的溶解度曲线研究对于药物的研发、生产和临床应用具有重要意义。
